|
11/27/2023 0 Comments Functions of synovial fluid 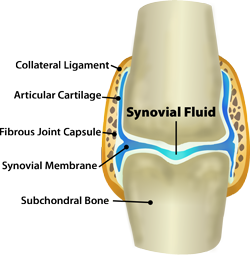
No basal laminae are separating lining cells from subintimal connective tissue and, unless inflamed, rare cell junctions. Type B cells show abundant rough endoplasmic reticulum. Type A cells show prominent Golgi cells, vesicles, vacuoles, lysosomes, and mitochondria. Neuropathic joints and rapidly destructive joint processes are characterized by bone and cartilage debris.įigure 72-5 Ultrastructure of synovial intimal cells. In septic arthritis, leukocytes are seen in tissue. Inflammatory arthritis (classically rheumatoid arthritis) shows a dramatically reddish hyperplastic synovium with fibrinous exudation characterized by abundant tan fibrinous loose bodies, called rice bodies, and marked lymphoplasmacytic synovitis. In general, traumatic synovitis and degenerative joint disease (DJD) (osteoarthritis) are attended by edematous change and mild villous hypertrophy. The villous appearance of synovium is not abnormal but is rather nonspecific and may be seen in a broad range of conditions ( Fig. D, Superficial zone foreign body giant cell reaction to a failed prosthesis. C, Mucinous hyperplasia illustrating the secretory potential of synovium. B, Hyperplastic synovium showing moderate hypertrophy of cells confined to the surface, with increasing hyperplasia and hyperplastic cells migrating into the subintimal zone with marked hypertrophy. Collagen is increased in the vicinity of dense connective tissue structures. A yellow color ensues with xanthoma cell accumulation, which may be a predominant feature of PVNS or xanthomatous disease.įigure 72-3 A, Normal synovium consists of a fine single or double layer of lining intimal cells on top of a subintimal zone of vascular and fatty tissue, fibroblasts, and rare histiocytes and mast cells. White foci in the synovium usually indicate gout (urate deposition), pseudogout (calcium pyrophosphate deposition ), or soft tissue calcifications (deposits caused by trauma or calcinosis syndromes). Darkening or blackening also may be seen with extensive release of metallic debris. In ochronosis (alkaptonuria), the synovium may appear a dull gray, whereas fibrocartilage and articular cartilage are discolored black. A reddish purple or rusty synovium indicates a hemangioma or bleeding and may be seen in trauma, bleeding disorders such as hemophilia, von Willebrand’s disease, and pigmented villonodular synovitis (PVNS). In cases of severe bleeding, a dark purple or rusty color may be noted. 72-2) owing to hemosiderin deposition and the release of iron from red blood cells. With hemorrhage, it becomes obviously bloody, but in chronic hemarthrosis, it turns a reddish or rusty brown ( Fig. Normally, the synovium appears smooth and transparent, but it turns thick, dull, and opaque with pathologic change. These structures histologically resemble normal synovium and often have demonstrably similar secretory and phagocytic functions. In pathologic states, synovial-like anatomic structures not related to a joint space (“synovial metaplasia”) are known to form in a variety of circumstances, including (1) postsurgical states (2) failed prostheses, including breast implants 29 (3) mechanical damage to connective tissue and (4) experimental settings (injected air or oil in subcutaneous soft tissue). The term joint capsule refers to the fibrofatty neurovascular tissue that envelops the nonarticular cartilaginous tissue of the joint space. Joint capsule fibrous connective tissue is thought to add to the joint’s mechanical strength. The extensive synovial-like lining cells of tendon sheaths and ligaments explain a host of reactive synovitis and painful clinical tenosynovitis, bursitis, and enthesopathy syndromes. 
Parietal and visceral synovium mimics their mesothelial-like counterparts in the thoracic and pericardial cavities. The synovial membrane, the most superficial layer of the synovium, lines the joint and forms the linings of tendon sheaths. In Vigorita VJ : Orthopaedic pathology, Philadelphia, 2008, Lippincott Williams & Wilkins.) Figure 72-1 Embryonic joint showing evolution of primitive mesenchyme (A) into a joint space (B) at about 8 weeks of intrauterine life. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
